Combating Vaccine Wariness With Education Here’s what philosophers, ethicists and medical experts say is missing
Published February 12th, 2021 at 6:00 AM
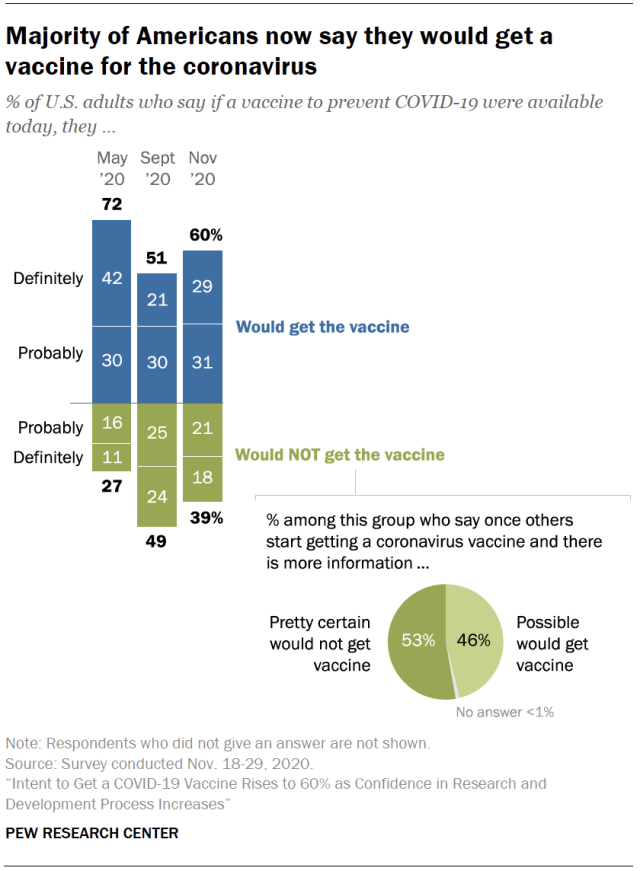
Above image credit: Data show that roughly 60% of the U.S. are willing to get the vaccine. What about the people who aren't sure? (Collage by Vicky Diaz-Camacho)Kiki Serna felt anxious before she got her first dose of the COVID-19 vaccine.
Serna, who works at the Mattie Rhodes Center, is healthy and young. However, her work is public-facing, involving a lot of community outreach for food drives, providing mental health support or processing rental assistance checks.
So, she signed up at KC Care Clinic to get her shot, but not without doing some research first.
“(I) wasn’t really questioning the vaccine. It was more so … having a lot of questions in general,” Serna said. “I was more so worried about the effects. Like if I got it, is it going to be painful?”
Serna got her first dose almost three weeks ago and went back for her second dose this week. Though she was nervous, she knew how it worked and what side effects to expect. What helped, she said, was doing research. She also had the chance to speak to a doctor — her uncle — who was among the first in Mexico to study the development of the COVID-19 vaccine.
“He kind of helped me calm my fears,” she said. “He’s my tio, but also he is a professional.”

Vaccine misinformation is pervasive in the Latinx community, where unfounded claims are shared through WhatsApp and forwarded on to family group chats. Barriers to solid information can incite panic about the pandemic and send the wrong message about the efficacy of the new vaccines.
The same goes for Native communities, said Rhonda LeValdo, who is Acoma. LeValdo recently received her second dose.
“Just like everybody else, I was apprehensive,” she said. “Being a person of color, Native Americans died through diseases that were brought here.”
Got my second shot! Feeling okay! pic.twitter.com/ZGdhjM3FRQ
— Rhonda LeValdo (@rhondalevaldo) February 3, 2021
But she feels fine, she said. Her side effects were mild. LeValdo, who is a professor at Haskell Indian Nations University and a journalist, said she was able to understand how vaccines work through firsthand research.
She’s interviewed Native doctors before to investigate anti-vaccination mentalities.
To her, getting the vaccine is the “sound choice.”
She added: “I just want to be able to see my mom, my grandma and my people.”
Data and Disparities
Missouri was recently listed as the fourth least vaccine-friendly state in the country, according to a What If Media Group survey.
In Kansas, 39.4% of respondents said they were unwilling to get the vaccine even if they were offered a $1,500 incentive. The online survey included 72,074 randomly selected adults in the U.S. and ran between Jan. 19-22.
Experts say people who are wary of getting the vaccine to combat COVID-19 might not have access to – or know how to find – credible information. Another hurdle is signing up for the vaccine. Some people don’t have easy access to technology.
The other problem has been distribution, as Flatland reported earlier this month. This in particular has been a problem in rural areas and some urban areas of the Kansas City metro.
In the Kansas City area, roughly 9% of the population is Latinx, 12% is Black and about 3% is Native, according to Census data. All of these populations have been hit hard by the virus, with higher rates of hospitalizations, health complications and death.
The most recent data analyzed by the COVID Tracking Project at The Atlantic shows just how hard.
In Kansas, Latinos were the most likely to contract COVID-19 and Native peoples were more likely to die. In Missouri, Latinos were also most likely to contract the virus and Black people were more likely to die.
The question is why? And where does the vaccine come into play?
According to several experts, lack of vaccine access, information – or misinformation – and distribution illuminate a deeper problem.
Countering Skepticism
Ruqaiijah Yearby, a professor at St. Louis University who is an expert in public health and law, said mistrust in the hospital system predates the pandemic.
Yearby wrote on vaccine skepticism among the Black community for The Appeal, which reads in part:
“Despite being one of the most affected and at-risk groups for COVID-19, Black communities remain largely skeptical about the vaccine. Rejection of this life-saving measure constitutes a huge risk to the Black community and the entire country, which requires an intensive national effort to confront and remedy it.”

Yearby, who is also the co-founder of the Institute for Healing Justice and Equity, said the pandemic highlighted the pre-existing structural issues in health care, government and the workplace.
She specifically pointed to government inaction, hospital maltreatment and lack of workplace protections.
One case in point, are meatpacking and poultry companies that did not act soon enough to provide Personal Protective Equipment (PPE), which could have prevented infection in the first place. As a result, more of their employees who are essential workers got sick.
“Whole communities have been infected and now you can give money for vaccines when you couldn’t help with a mask or free tests?” Yearby said.
In the current context, she added, workers who do not have paid sick leave might opt out of getting the vaccine because of the side effects. Workplace structures also have a part to play in how communities respond. Simply put, some people cannot afford to take an unpaid day off.
These disparities should not be seen as a cultural or biological difference, she added. It’s “quite clearly a structural issue.”
This also applies to outreach, which keeps overlooking vulnerable communities.
“The vaccine rollout cannot be disconnected from the need that people have in their daily lives,” Yearby said. “Some of the same structural issues that have prevented people from staying home when they’re feeling sick is the same thing that prevents them from standing in line to get the vaccine.”
Yolonda Wilson, a philosopher whose research focuses on bioethics, race theory and social and political philosophy, echoed Yearby.

She pointed to structural injustice, which has historically hurt communities of color.
“I think being really intentional about access to information should matter. And a lot of places … there’s an assumption of literacy,” Wilson said.”
Assumption of literacy includes English, access to the internet or a computer, and transportation, among other things. Sign-up forms for the vaccine are mostly online, asking folks to enter their email addresses.
The next best thing is to call.
But Wilson said she tried calling to get information on how to get the vaccine herself. Nobody picked up.
“Any rollout plan has to think about how people actually live and not just people with money and resources,” Wilson said.
“When I think about structural injustice these are the kinds of things I think about. You don’t have to be English-speaking or tech-savvy in order to be healthy.”
Jason Glenn, professor of history and philosophy of medicine at the University of Kansas Medical Center, agreed.
Glenn has been working on distribution and figuring out the vulnerability index at the Unified Government of Wyandotte County and Kansas City, Kansas, Health Department.
“We faced the problem that state allocations of vaccines have kind of been shortchanging the counties, in favor of a lot of the medical centers,” he said. “We’re trying to correct that.”
Glenn added: “What’s most troubling to me (is) we seem to be suffering from the twin issues of rampant misinformation that there is out there about vaccines in general that predated the coronavirus.”
In addition, poorer communities and communities of color are more predisposed to higher infection rates. He attributed the predisposition to the higher amount of toxins that people of color are exposed to due to housing discrimination and type of labor.
“We know that the stress of discrimination adds a lot of wear and tear on the bodies,” he said. “What that means for us is that we have higher disease prevalences as well. It just so happens that the higher disease prevalence that we have, the coronavirus loves to just eat those up.”
For this reason, the vaccine is particularly important for communities of color.
“When you’re thinking about getting the vaccine, you should not just be thinking about, you know, yourself,” he urged.
Part of Glenn’s work has been to poll community members and hear their concerns. Those range from rumors of government interference or whether one can catch the virus from the vaccine.
“All of those things are not true,” he said.
One of the main issues people are concerned with is the speed at which the vaccine was created.
“Although it seems like this vaccine was developed in a very short period of time, the technology that it uses – the messenger RNA technology – has been in development for over 30 years,” he said.
This work is credited to Turkish-German immunotherapy specialists and spouses, Ugur Sahin and Özlem Türeci. They used mRNA technology in cancer treatment “to trigger the production of certain proteins in cells, which could then train the immune system to attack cancer cells,” according to the BBC.
Or, as Glenn explained: “(The vaccine is) wearing a jacket with the virus logo on it, but there’s no actual virus inside. That teaches the immune system to attack anything that looks like that without actually exposing you to the risk that you might catch the disease.”
Back to Basics
Health literacy – and access to it – has been on the back burner for some time.
At least this is what Brenda Linares has observed.

Linares is a medical librarian in the school of nursing at University of Kansas Medical Center. Her work has largely focused on the Latinx/o/a community and the prevalence of misinformation.
She is also part of JUNTOS, a health initiative focused on bridging the gap of information and providing robust health literacy training for Latinos in the Kansas City area.
“That’s something that is really unfortunately low when it comes to minority populations,” Linares said. “A lot of them have not had much schooling or training. They … search, find something, and then (think), ‘This looks legit, they have a website, they have nice visuals.’”
That’s why outreach is key. Lack of resources and funding means communities of color aren’t being educated as well about the vaccine, how it works, and, more generally, about where to get it and why.
Even Linares struggled to find information to sign up her 65-year-old father who lives in Johnson County. This information was all in English.
Linares wanted to share the COVID information chart with her parents, who are from Guatemala but instead had to translate it to Spanish herself.
“I think there’s a lack of communication,” she added.
This only feeds the confusion.
Additionally, she said, some of the people she’s worked with, for example, come from places where governments were abusive. So when they arrive in the U.S., they are already wary of government entities, public health officials included.
Education can help combat bad information, she said, and ensure that communities are getting the health care they need.
As a librarian, Linares said education can start with figures people trust most at community centers and even churches. But keep the information simple and straightforward, she added. That includes educating on how the body works, or how the body gets infected with the virus. Then explain how the vaccine can help.
Not everybody understands that.
“You need to go (back to) the basics,” she said. “Having those conversations is really important.”
Correction: An earlier version of this article misspelled Ruqaiijah Yearby’s name.


