An Olathe Hospital Sued Thousands for Medical Debt, and Dozens Went to Jail Precarious Balance of Cost and Compassion in Health Care
Published July 8th, 2020 at 6:00 AM
Above image credit: Olathe Medical Center and Emergency Medicine Care officials say they are making changes to help patients, but they are still suing more patients in court for unpaid bills than neighboring health systems. (Jeff Tuttle | The Journal)Haley Graves was running across the deck of her family’s home in 2018 when she hit a patch of ice and went down on her right arm, breaking it in two places. Her mother, Debbie Graves, packed her injured daughter into her car for the five-minute drive to Olathe Medical Center.
A year and a half later, the hospital sued Haley for being late on payments and summoned her to court. Haley, a 24-year-old woman who has autism, burst into tears when she learned about the summons. “She thought she was going to jail,” Debbie Graves says.
It won’t come to that for her, but the notice was the start of an ordeal that thousands of people in and around Johnson County can relate to: For patients who have run up charges at Olathe Medical Center, its emergency room and other associated health facilities over the past six years, the health system and its ER physicians group go to great lengths to collect overdue bills.
Other hospitals sue patients in Johnson County. But before the COVID-19 pandemic shook up daily life and shut down courtrooms, none did so as frequently as Olathe Medical Center. The hospital’s emergency room physicians, who operate a private company called Emergency Medicine Care LLC, have, until recently, used the court system even more frequently to collect on unpaid bills from their patients.
Occasionally patients with unpaid emergency room bills wound up in jail. That happened at least 60 times in the past six years, court records show. Those patients were arrested on bench warrants for contempt of court after they were sued and subsequently failed to appear in court. The bonds they posted to get out of jail were then applied to the debts they owed to Emergency Medicine Care.
That happened to one patient interviewed by The Journal, Tracy Burford of Olathe, who was jailed in January after missing a fall court date. The $250 bond she paid to secure her release was paid to Emergency Medicine Care to resolve a judgment for several hundred dollars against her. When she was late to court again a week later, the judge issued another bench warrant, this one carrying a $500 bond.
After receiving questions from The Journal about the practice of using bench warrants, the physician who serves as president of Emergency Medicine Care, Dr. Shawn Stanley, said in a statement that the group has instructed its legal representatives to stop issuing them as “the final step in their collection process.” Olathe Medical Center’s financial assistance policy had already spelled out that it doesn’t seek arrests as part of its collection efforts, but that didn’t cover care through Emergency Medicine Care, which is a separate entity.
One practice both providers share is the use of garnishments to collect on unpaid bills. When court summonses and collection notices don’t get results, lawyers representing Olathe Medical Center and Emergency Medicine Care have sought garnishments, in which money that would otherwise belong to the patient – such as a paycheck or a bank account – gets paid to a creditor instead, often in increments. Between 2014 and 2019, health system patients were involved in about 800 garnishment cases, and at least 2,200 garnishment cases involved ER patients across the Olathe Health system, a Journal analysis of Johnson County court records show.
The garnishments affected dozens of employees at workplaces such as Walmart and the Olathe School District. In at least 38 instances, attorneys for the hospital or ER doctors group sought garnishments from employees of Olathe Medical Center itself.
Ashley Pierucci says her biweekly pay from the Olathe School District, where she worked as a paraeducator, dropped by about $75 last year because of a garnishment, leaving her with barely enough to pay bills and take care of her two young daughters.
Pierucci says the charges stem from bills incurred during her second pregnancy, when she was covered by KanCare, the Kansas Medicaid program, which provides health coverage to some Kansans with little income. “I tried fighting it, and it was never resolved, so they sued me,” she says.
The hospital’s financial assistance policy indicates that patients who have documented Kansas Medicaid eligibility within the previous six months and who meet residency requirements will be presumed eligible for a discount of 100%. Hospital officials did not provide an explanation as to why Pierucci and other patients who report being on Medicaid would not presumptively be eligible for aid.
With her paycheck reduced, Pierucci found herself juggling expenses. “I have to alternate paying some bills,” she says. “I’ll be late on one bill, and next month I’ll pay it on time and pay another bill late. Just trying to make it work.”
Court records show Pierucci owed about $1,500 at the time her paycheck was garnished.
“I mean, if that’s the only way I’m able to pay them that’s fine,” she says. “But I wish I had more money in my pocket to do stuff with my girls.”
Hospital officials and their attorneys defend the lawsuits as a last resort when all other methods to resolve unpaid bills have failed. In a statement to The Journal, they indicated that they have been making changes to benefit patients struggling with unpaid bills, including providing alternative payment options and increasing the minimum balances on which they will try to collect.
“At Olathe Health, we continuously review our systems and procedures regarding financial assistance to make sure they are best serving our patients. Over the past three years, we have implemented changes to improve our financial assistance program, and recently updated our collection actions,” a statement from hospital spokesman Mike Jensen said.
But the challenges of dealing with medical debt in Kansas, one of 14 states that has not yet expanded Medicaid eligibility to cover more low-income residents, might only get more complicated. The pandemic that puts health workers across the state, such as Stanley and his colleagues, in harm’s way also devastated the budgets of hospitals that, like Olathe Health, suspended elective procedures and outpatient visits in service of halting the spread of the virus and preparing to treat those affected by it. With the economy and the courts reopening amid high unemployment and hospitals in a weakened financial position, should more patients be worried about finding themselves in court if they can’t pay for their care?
After all, when the economy was roaring, medical debt still proved to be a widespread problem, even in Johnson County, where the median household income prior to 2019 was $84,915 a year. Survey data from the Urban Institute showed about 13% of county residents reporting having medical debt in collections as of 2019, with an average debt of $1,422.

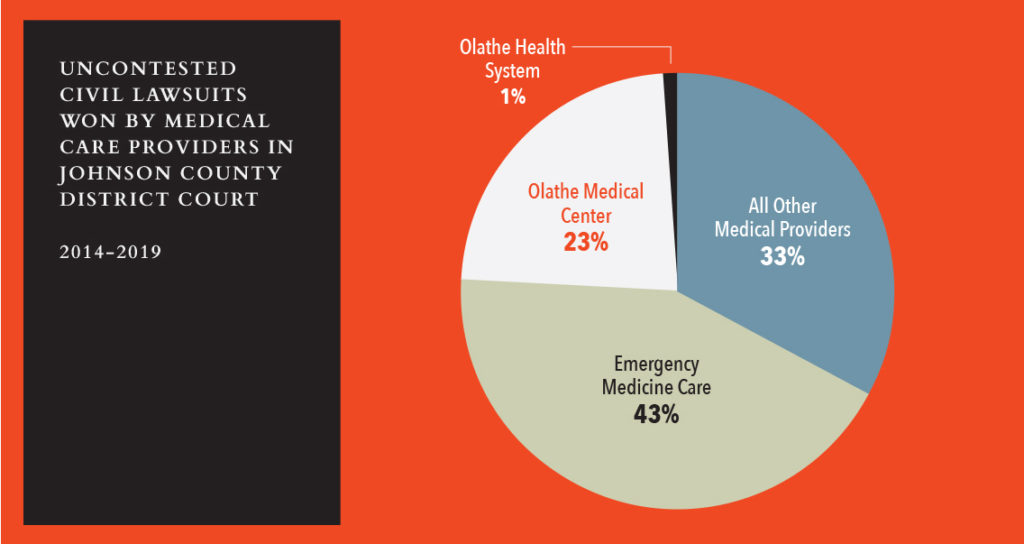
Yet not all providers use the courts to collect unpaid bills to the same degree. Between 2014 and 2019, Emergency Medicine Care and Olathe Medical Center accounted for about two-thirds of all uncontested collection lawsuits won by medical care providers pursuing limited civil actions in Johnson County District Court, The Journal’s research shows. Every other identifiable hospital, medical center, physicians group and health system combined – about 280 different providers in all – account for the remaining third. Uncontested judgments occur when a defendant fails to adequately respond to a lawsuit and are a common outcome in medical debt collection cases. They frequently lead to creditors enlisting the help of the court to collect what they’re owed through garnishments.
The situation in Olathe is a window into how institutional policies and practices can have deleterious effects on the lives of low-income and working-class Kansans even in the wealthiest of places. It’s a civic challenge that permeates other aspects of life in Johnson County and beyond, from housing to transportation to the criminal justice system.
The Journal began looking into medical debt collection by nonprofit hospitals in Johnson County after ProPublica, a nonprofit newsroom that produces investigative journalism in the public interest, shared reader tips last November about medical debt collection practices in Kansas.
Stanley notes that Emergency Medicine Care underwent a shift in leadership in July 2019, and a Journal analysis of Johnson County court records shows that the group’s debt collection activities in court slowed considerably beginning that year.
In a statement, the group emphasized Emergency Medicine Care’s focus on providing “expert compassionate care to patients and families of the Olathe Health System.
“We have done this in the setting of a global pandemic and unprecedented economic shutdown, all while focusing on the safety of our patients, nurses, supporting staff, and ourselves,” the statement said. “We have treated the most critically ill, often while those same patients were fully isolated from their loved ones. We have had to isolate ourselves at times from our own families due to this pandemic. This is our profession, and we will continue to provide the most complete, compassionate care to our patients as this pandemic continues.”
Olathe Medical Center spokesman Jensen also referenced the hospital’s role in helping respond to COVID-19, saying that since the pandemic began “our number one priority has been the safety of our patients, associates and providers, fulfilling our mission to help people through healing, health and happiness.
“During this time, the priority for our debt collection and financial assistance departments has been on how we can best accommodate our patients who have been financially affected by the pandemic,” the statement said. “We have altered our financial assistance and debt collection policies to accommodate patients dealing with financial hardship.”
Those changes include: providing additional charity care for patients who now qualify due to job loss or the loss of health insurance and offering extended payment plans and lower monthly payments. Jensen also noted that collection attorneys representing the health system suspended all court action in March when the pandemic started.
“Any resumed Court actions will be with consideration for pandemic-related circumstances and in conjunction with the Court’s operations and directives,” the statement said.
How hospitals such as Olathe Medical Center choose to deal with medical debt after they care for patients, however, likely matters now more than ever. Amid rising costs for care, patients are being asked to cover more of their own health care costs through higher premiums, deductibles and copays. Although more Kansans gained health insurance after President Barack Obama signed the Affordable Care Act (ACA) into law a decade ago, about 8.5% of the population remained uninsured in 2017, according to the Kansas Health Institute, and those who do have coverage are frequently paying more.
But with about 10% of Kansans out of work and more than 100,000 qualifying for unemployment benefits, an untold number of workers almost certainly have lost their health insurance. In Johnson County last month, the unemployment rate stood at 9.3% after being just 2.6% the previous May, according to the state Department of Labor.
As many as 137 million Americans are struggling with medical debt, according to the Journal of Internal Medicine. In places such as Johnson County, where housing costs are high and 28% of jobs pay less than $15 an hour, there was a sizable population struggling to keep up with daily expenses even before pandemic-related job losses.
Multiple research studies published over the past 15 years have documented how patients struggling with medical bills are more likely to defer care or not return to their doctor, decisions that have implications for their long-term health.
Serving patients who can’t afford to pay has traditionally been a role that nonprofit hospitals have filled and is one of the reasons they’re exempt from taxes. But a handful of nonprofit hospitals around the country have faced scrutiny in recent years for aggressive debt collection practices. Some of those hospitals engaged in practices similar to what Olathe Medical Center patients report having experienced. The scrutiny has prompted some, but not all, institutions to reevaluate or change their policies.
Olathe Medical Center officials say their collection practices are in accordance with Internal Revenue Service regulations and that they “exhaust several attempts to accommodate a patient’s financial needs before the account is turned over to a collection agency.”
In recent months, the system says it has also increased the minimum pursuable action to $750 from the previous threshold of $500. Jensen, the health system spokesman, said that hospital officials believe the higher minimum will ultimately decrease the number of cases Olathe Health sends to court.
But court records show the health system is still pursuing a significant number of legal actions in 2020. The number of uncontested collection lawsuits won by the health system reached a six-year high of more than 600 in 2019. Olathe Health entities filed more than 300 limited action civil lawsuits through the end of May and won more than 170 uncontested judgments, even though courthouse operations were disrupted by the COVID-19 pandemic and hearings moved online. Emergency Medicine Care filed 100 lawsuits of its own and won 32 uncontested judgments. No other creditor won more than 91 uncontested limited action judgments over the same period, online court records show.
The ACA added some requirements that nonprofit hospitals have to meet to retain their federal tax-exempt status. But hospitals such as Olathe Medical Center still have latitude to determine what they charge patients, what discounts and financial assistance to offer, as well as how to respond when a patient doesn’t pay up. Patients often face the prospect of receiving multiple bills from different providers who may care for them at the same location, sowing the potential for confusion. A Kaiser Family Foundation survey indicated that Kansas is one of the nation’s five worst states for surprise medical bills.
The situation raises leadership questions about how nonprofit hospitals such as Olathe Medical Center should balance being fiscally responsible and dealing compassionately with patients’ debts. Are hospitals making life for their patients – particularly those with the least ability to pay – better or worse? What responsibilities do patients themselves have? And what should state and community officials be doing to blunt the harm of such a pervasive problem?
A 2017 community health access survey paid for by philanthropic health foundations in Kansas and Missouri (including the Kansas Health Foundation, funder of the Kansas Leadership Center, which publishes The Journal) showed that 28% of adults ages 19-64 in Kansas and 33% of children 18 years old and younger live in households that struggled paying medical bills over the previous year. At the time the survey was released, foundation officials told reporters that medical debt and a lack of insurance were “financially crippling families” and preventing them from getting the treatment they need.
A ‘night and day’ difference
The Graves family found the process of working out their bill with Olathe Medical Center stressful, even humiliating.
The initial statement Debbie Graves received for treatment of Haley’s broken arm was $31,000. Without explanation, that amount was reduced to $14,000. Court records show that Haley’s charges were adjusted downward because she was uninsured. Under the ACA, hospitals aren’t supposed to charge uninsured patients any more for a service than they would private insurers or a government insurance program for medically necessary care. And they’re supposed to do this before factoring in discounts or write-offs for financial assistance.
But the lower bill was still far out of reach for Haley’s family.
Because of her autism and related sensory issues, Haley is unable to work, her mother says. She receives an allowance from her parents and makes a few dollars selling clay figurines and jewelry on an Etsy shop, HevanlySprings.
“She has $20 to her name right now,” Debbie Graves says. “What are they going to do with that?”
Graves and her husband, Michael, operate a small nonprofit faith-based organization, My Father’s House Ministries. Among other services, they provide birthday cakes for children in detention centers, shelters and other tough situations. And they grow organic produce to assist agencies serving Johnson County’s growing homeless population.
To meet living expenses, the family relies on personal gifts from friends and people who support their ministry, and income from two adult sons, both of whom work in supermarkets.
When it came to paying the bills for Haley’s injury, the family was on its own.
Haley and her parents have no health insurance. Because of their unusual income structure, they are unable to qualify for a subsidy under the Affordable Care Act, Debbie Graves says. Kansas’ Medicaid limits exclude most adults from coverage, and the Legislature has refused to join the majority of states in expanding eligibility.
“We’re just like a lot of people,” Graves says. “We’re living month to month. We have no retirement, no health care, zero savings.”
Graves says she visited a patient financial services office at Olathe Medical Center, hoping to work out a payment plan. A woman queried her about the family’s sources of income, she says. Graves says the woman told her to look for a “welcome pack” in the mail, with a payment proposal.
She never received any communication from the hospital, Graves says. But she did receive multiple not-so-welcoming letters from a law firm retained by the hospital. After the hospital sued, her mother hired a lawyer, Jordan Schwartz, who represents defendants in debt cases.
“Thank goodness for Mr. Schwartz, because we didn’t know anything,” Graves says.
Schwartz says he has represented many clients being sued by Olathe Medical Center and its entities. Many are on limited incomes and think they can let their hospital bills slide, he says. They are surprised to find themselves in court, sometimes over relatively small amounts.
His role, Schwartz says, is to negotiate with the hospital’s attorney and work out a payment plan. Usually his clients pledge to make monthly payments, and the medical groups agree to stay the interest on the debt. As long as the client makes payments, the hospital will refrain from garnishing patients’ paychecks or bank accounts.
That’s the deal Schwartz worked out for Haley Graves. After the hospital’s attorney refused Schwartz’s entreaties to reduce or forgive the debt, the family agreed to pay Olathe Medical Center $50 a month indefinitely. For both sides, it seemed the best they could do. Assuming she’s able to make all the payments and avoid interest costs, Haley will be free of the debt in slightly more than 23 years under the payment schedule.
Debbie Graves says the collection notices and court summonses caused her sleepless nights.
“I thought someone in the hospital would say something like, ‘Look, Haley’s uninsured. She’s disabled. Maybe we can get you some help,’” Graves says. “Not that it matters, but it hurt my feelings to be treated like rubbish, instead of like a human being.”
In what turned out to be a painful but revealing coincidence, Michael Graves got knocked down by an overly enthusiastic puppy in January and broke his left arm.
Ignoring the grotesque sight of her husband’s dislocated wrist and twisted hand, Debbie Graves drove straight out of Olathe and headed for AdventHealth Shawnee Mission, a hospital 10 miles farther away than the trip she’d made with Haley.
“When they found out Michael was uninsured, they went to great lengths to try to help us,” Graves says. “I called them when I got the bill in the mail. I said, ‘Look, I can’t pay the whole thing up front.’”
In a single phone call, Graves says, a representative offered her a two-year payment plan in which the hospital would automatically withdraw a reasonable amount each month from the bank account she shares with her husband. There were no collection notices, no court summonses, no tears.
“No problem at all,” Graves says. “They were kind and considerate. It’s not like we don’t know that people need to get paid. We just need a way to do it. The difference between Shawnee Mission and Olathe, for the same injury, really, was night and day.”

How some with unpaid medical debt wind up in jail
The pursuit of unpaid bills can result in patients facing consequences that go beyond simply being hounded to pay what they owe. When patients have judgments placed against them, they often end up owing interest accumulated before the judgments as well as paying for costs that plaintiffs incur in bringing their cases to court. Many patients also face the prospect of paying a 12% annual interest rate on their debts after the judgments, which is an amount set in state statute.
There can be severe consequences for those who don’t show up in court when ordered to do so. Tracy Burford of Olathe found that out when she was pulled over for a traffic violation. The officer told her there was a warrant out for her arrest. The charge: contempt of court.
Burford, whose sole income is a monthly $734 disability check that cannot be garnished, had failed to appear in court for a hearing to explain why she had not satisfied a judgment against her. The judge had issued a bench warrant, with a $250 cash bond.
After spending six hours in jail this past January, Burford used money she had saved up to pay other bills to bond herself out. The $250 went toward the judgment obtained by Emergency Medicine Care.
Burford says she has colitis, a chronic inflammatory digestive disease. It is the reason she receives disability payments and also the cause of frequent visits to the emergency room or a clinic. She says she has Medicaid, but some expenses aren’t covered.
After her stint in jail, Burford was given a new court date. She says she was coping with an intestinal flareup that morning and arrived late. A lawyer then told her the judge would issue another warrant for her arrest, this time with a bond set at $500.
All of this had been precipitated by a debt of about $400. She said she didn’t know what she would do about the new warrant. More than five months after it was issued, the warrant has not yet been executed, court records show.
“If I had money for anything, I would have paid my bill to begin with,” Burford says.
ProPublica reported last year that patients in Coffeyville, in southeast Kansas, were being arrested under similar circumstances. Burford’s arrest shows that similar medical debt collection practices happen elsewhere in Kansas. Between 2014 and 2019, at least 60 Emergency Medicine Care patients were arrested after missing court appearances, bonded out and had their bonds applied to the judgments against them. The arrests occurred after attorneys for Emergency Medicine Care requested that a judge call debtors into court because creditors were having trouble collecting.
The figure could have been higher. The Journal’s analysis of Johnson County court records shows that attorneys for Emergency Medicine Care prepared contempt citations to be served on ER patients in more than 500 cases between 2014 and 2019. Those patients often appeared in court and avoided a warrant.
When it was queried on that practice – and how it differed from Olathe Medical Center’s – the physician group took a step back.
A statement from Stanley, of Emergency Care LLC, said the group relies on a third-party collection agency, Account Recovery Specialists Inc., with offices in Wichita and Dodge City. The company is known by the acronym ARSI and is used by other Kansas hospitals in collection actions, including Olathe Medical Center since late 2018.
“Our management team adamantly affirms that it has not provided ARSI with any directive or instruction to be any more aggressive with collections efforts,” than the nonprofit hospital, the statement said. “EMC was unaware that its patients purportedly faced more lawsuits and garnishments than patients who owed their debt to the nonprofit hospital prior to your (The Journal’s) letter. … We have full intention for the companies that manage our billings and collections to take a compassionate and fair approach to these challenging situations.”
The statement referred additional questions about Emergency Medicine Care’s collection process to Joshua Shea, the general counsel for ARSI. In an emailed response to questions, Shea described Olathe Medical Center as “an extreme outlier” among plaintiffs, including other ARSI clients like Emergency Medicine Care, because it doesn’t seek contempt citations if a debtor fails to appear at a hearing to disclose financial information.
Emergency Medicine Care “like almost every other plaintiff who files lawsuits and like the overwhelming majority of ARSI clients, had not asked for the legal process to be halted prematurely with there being no post-judgment step following” a no-show for a debtor’s exam.
“With your recent questioning of them and informing them of what” Olathe Medical Center has in place, Shea said the ER physicians group asked ARSI and the attorneys it works with to “preclude the court from issuing contempt citations while they assess how to make sure” that the two entities largely share the same collection practices.
In a subsequent statement released June 21, Emergency Medicine Care indicated it has continued implementing CarePayment, a health care financing program also used by Olathe Medical Center that offers patients options for paying their bills over an extended period of time.
“The process has continued and no accounts have been sent to ARSI for collections since the onset of this process in February,” the statement said. “With the broad economic shutdown and widespread hardship ARSI was instructed by our group to halt all collection inquiries on existing accounts in early April. ARSI developed their own policy with the cessation of all collection practices extending for 90 days.”
Although the group did not respond to The Journal’s request for a written copy of its collection and financial assistance policies, the statement said that, “Emergency Medicine Care has and will continue to fully align our collection practices with that of Olathe Health.”
Olathe Medical Center and Emergency Medicine Care have sought garnishments to collect at least $3.4 million combined in unpaid bills since 2014. However, that figure only includes judgments posted in the district court’s publicly available online summary of case activity and does not factor in all the fees and interest being charged. It’s also not clear from court records how much has actually been collected. Of the judgments recorded publicly, the average debt being pursued was about $2,500 for Olathe Medical Center and about $850 for Emergency Medicine Care.
Court records indicate that uncontested judgments account for only a portion of the legal activity involving Emergency Medicine Care and Olathe Health in limited action suits. Using the “partial name search” function on the Johnson County District Court’s records website, The Journal found Emergency Medicine Care listed as the plaintiff in more than 5,900 limited action cases filed between 2014 and 2019. Olathe Medical Center was listed as the plaintiff in another 4,000 limited action cases over the same period. Representatives of Emergency Medicine Care and Olathe Health declined to specify how many collection lawsuits they had filed over the past six years.
Some critics argue that more aggressive debt collections are bad not only for patients but also for the hospitals that engage in them, at least over the long haul. Trying to squeeze money out of patients who struggle to pay, they say, does little for a hospital’s bottom line and could further trap struggling patients in a cycle of debt that makes it harder for them to pay off future hospital bills. Not every hospital engages in frequent court actions, and some are foregoing lawsuits more often in favor of working directly with patients to resolve their bills.
Because Kansas courts have only gradually begun to resume normal operations, it’s too early to say whether pandemic-related financial pressures will lead to more legal action by Olathe Medical Center and other hospitals. But such practices were hardly universal before the pandemic.
When researchers studied garnishments related to medical debt in Virginia, they found that nearly two-thirds of hospitals there did not seek garnishments, according to a research letter in the Journal of the American Medical Association. A small number of hospitals, four of five of which were nonprofits, were responsible for 51% of all garnishment cases there.
Shea of ARSI argues that his clients only sue after they have run out of all other options. He notes that 84% of Kansas hospitals had a negative operating margin. And that figure was before the pandemic.
“Ultimately what we have here are service providers who have gone unpaid for their work and that exhaust efforts to be paid something over some period of time or to be able to grant financial assistance or charity care to those in need,” Shea wrote.
The ways to reduce the number of lawsuits that hospitals such as Olathe Medical Center are filing, Shea says, include expanding the state’s Medicaid program to ensure more low-income Kansans receive health coverage. He went on to say that members of the media such as The Journal could also better encourage awareness among consumers of the financial assistance and charity and extended payment options that exist among medical providers.
“I would disagree that a solution is for service providers, of any type, to go unpaid,” Shea wrote.
But when patients get sued, it leaves an impression. Haley Graves and more than a dozen other patients or relatives of patients told The Journal they won’t soon forget the emotions that were churned up when they learned they were being sued by Olathe Medical Center or Emergency Medicine Care.

‘I can’t afford this’
Barring shutdowns for pandemics and other emergencies, dozens of people file into Room 222 of the Johnson County Courthouse every Thursday morning for the “answer docket,” involving what is known in the legal trade as Chapter 61 actions. Journal reporters sat in on several of these dockets during the months of January and February, when the courts were operating normally.
The largest share of those present those days were defendants who received a summons telling them that a creditor had filed a legal action against them to collect money that they allegedly owed. Many weeks, a hefty percentage of the complaints came from Olathe Medical Center and its health network and emergency room provider.
The stories people brought to court were ones of injuries, illnesses, divorces and lost jobs – reasons why they had not and could not pay the debts that brought them there. But those stories don’t matter that much in court. Under Kansas law, hard times and tough circumstances aren’t enough to escape responsibility for paying one’s bills.
On a typical Thursday, Magistrate Judge Daniel Vokins listens as defendants get an opportunity to respond to the plaintiffs’ allegations. The court gallery is usually filled with about 50 people. Some defendants come with friends or family.
On the other side of the bar stand several lawyers representing clients who are attempting to collect money owed them. The docket usually lasts about half an hour and consists largely of the lawyers calling out names of defendants to see if they were in the courtroom.
Vokins tells defendants they can admit or deny what’s in the complaint. In a debt collection case, the complaint is straightforward: The plaintiff says it provided goods or services, and the defendant didn’t pay for them. Defendants who deny what’s set out in the complaint are advised by the judge to find a lawyer, or at least study up on Kansas civil law and provide a detailed answer to the complaint within 14 days. If they admit the debt is theirs, Vokins enters a judgment in favor of the plaintiff.
In either case, he advises defendants to talk to the lawyers representing the entities that are suing them. Perhaps they can work something out.
Lawyers and defendants file out of the courtroom and into the hallway. That’s where the real action takes place.
On a Thursday in January, at least a dozen of the people milling around the hallway were being sued by Olathe Medical Center. They trailed along as a pair of lawyers led the way down a staircase and a long hallway into a room usually reserved for jury pools.
The lawyers handed out clipboards with forms on which defendants were expected to disclose the details and status of their employment, marriages, housing situations and sources of income.
Lawyers and defendants then huddled for brief conferences to see if a payment plan was feasible. “Could you afford $50 a week? How much could you pay? When do you expect you’ll find a job?”
Elvira Lemus walked out of the jury room steaming. A baby in her family had been treated at Olathe Medical Center for respiratory trouble, she said. The family had expected Medicaid to cover the child’s expenses. When a $750 bill arrived, Lemus sent the hospital a letter with a copy of the child’s Medicaid card. The next communication she received was a summons taped to the family’s door three days before Christmas.
In the jury room, a lawyer representing the hospital told her to try to work matters out with KanCare, the program through which Kansas administers Medicaid. But she only had two weeks to do so. After that the hospital would pursue measures to collect the $750 it said the family owed.
Whatever the outcome, Lemus says she’s certain of one thing. “We’ve always used that hospital,” she says. “We will never go back.”
On another Thursday morning, three women with hospital-related cases waited outside the courtroom to talk to a lawyer. This time there were no clipboards and no chairs. All three women sprawled on the floor to complete their forms.
One of them, Gina Andrew, says Olathe Medical Center was already garnishing 25% of the paycheck she earns as a preschool teacher for an unpaid balance of about $2,000, incurred when she visited the hospital with severe abdominal pains.
Now Emergency Medicine Care was suing her for bills that court records show amount to about $800.
“I’m on my own,” Andrew says. “I can’t afford this.”
When contacted recently, Andrew, 33, said she’d been laid off from her job, which paid about $14,000 a year, because the preschool had shut down due to the coronavirus. She receives unemployment benefits, which the hospital can’t garnish.
Andrew said she’d racked up her medical bills while going through a rough patch, and along with intestinal problems, she broke a finger. When that happened, she went to Overland Park Regional Medical Center, a for-profit HCA Midwest hospital.
“They worked with me,” Andrew says. “They were a lot better to deal with. I haven’t been back to Olathe Medical Center. If I’m on my deathbed, I won’t go back there.”
Natasha Tarrant appeared in court the same day as Andrew. She had spent a few days in Olathe Medical Center for high blood pressure soon after the breakup of her marriage, during which she lost her job and health insurance. Now she’d been summoned to court for an unpaid balance of $359. But with medical bills upward of $15,000, Tarrant feared more to come.
In a brief conversation, a lawyer representing Emergency Medicine Care queried her about her progress filling out job applications. Tarrant figures any future paychecks will be garnished.
“As soon as I get a job, it’s all going to disappear,” she says.
“This is a foreign situation for me, because I was doing fine before all of this,” Tarrant says. “I do feel guilty about not paying, but at the same time, it’s so extremely expensive.”
For other defendants, being called to court is stressful even when it’s not financially catastrophic. On another Thursday in February, defendant Dana Nelson says she was insured when she had surgery at Olathe Medical Center in 2017. She called the hospital and, later, collections attorneys, to contest a bill of about $900. No one called back. “I figured it was reconciled,” Nelson said.
Then she received a notice summoning her to court. By the time she got there, she had already paid the late amount.
“It creates a lot of stress and anxiety,” Nelson says. “We pay our bills.”

The judge’s view
The process for a defendant to wind up in Vokins’ court can happen quickly, say as few as four to six months from a time a bill is first due, or take years. Under Olathe Medical Center policy, “extraordinary collection actions” such as lawsuits are not initiated by the medical center until 120 days after the date of the first post-discharge bill. The medical center generally accepts financial assistance applications up until 240 days from the date of the first post-discharge bill.
Regardless of how they get there or how long it takes, once patients find themselves appearing as defendants in court, plaintiffs have a variety of tools at their disposal to compel patients to cooperate.
Hospitals, or any creditor for that matter, have up to five years to issue a summons. During that time, they may resend their bills or send collection letters, possibly from a credit agency. Eventually, if a patient still hasn’t paid, he or she could find a summons to appear in court taped to the front door, personally delivered or sent by registered mail. The summons orders a defendant to appear at a specific time, with this warning: “If you do not appear before this court or file an answer at such time, judgment by default will be taken against you for the relief demanded in the petition.”
Despite that, the majority of cases go uncontested. Of the 12,000 cases Vokins hears every year, he estimates that about three-fourths of the defendants never appear in court.
Because of the pandemic, Vokins says he had to postpone his Thursday dockets from mid-March through May 11 before he came up with a solution as to how to conduct his hearings. As of May 18, limited action cases are being heard through BlueJeans Video Conferencing, with about 30 or so people appearing with each docket.
The only substantial change is that the debtors now supply their answers to questions about their finances in writing because it was hard to keep information confidential with video conferencing.
Case filings decreased when courts adopted remote proceedings, Vokins says, and he estimates he’ll be caught up on the backlog of cases by the end of June.
“From comments made from the collection attorneys, they indicated that some of their clients are holding off from filing lawsuits until the stay-at-home orders are rescinded, and on cases previously filed, they have some clients who do not want to take default judgments,” Vokins wrote in an email. “It appears the creditors are trying to work out payment arrangements, which I have encouraged attorneys to do.”
Still, it’s important to remember that there’s no law that requires communication by the time legal proceedings reach this point, just as there is no law that requires the plaintiffs and defendants to formally negotiate with a professional mediator. But Vokins encourages both.
“One complaint I’ve heard from debtors is they try to get information from attorneys by calling offices and can’t get a return call,” Vokins says. “I’ve encouraged the attorneys, ‘Look, communicate and see if you can work something out.’ ”
The avenues that patients have for not paying a bill once they are in court can be limited. Some defendants can dispute the amount or, in the case of a medical debt, argue that their insurance has failed to pay a bill covered by their policy. Some may claim that their medical provider failed to perform the correct service. But often, Vokins says, defendants will say they simply can’t afford to pay the debt.
“That’s not a legal defense,” he says.
Furthermore, few defendants in Vokins’ court get an attorney at any stage of the process.
Casey Johnson is assistant managing attorney at Kansas Legal Services in Wyandotte County, a nonprofit organization that offers legal advice and representation to low- and moderate-income Kansans. He says that people occasionally contact him for legal help with debts, medical or otherwise, but not often. “A lot of times when I do, it’s after the fact,” Johnson says.
“After the fact,” Johnson says, often means that the defendant has received notice that their wages are being garnished. At that point, the best that an organization like Kansas Legal Services can do is educate its client.
This is what its lawyers will say:
- Kansas law allows creditors to garnish up to 25% of a debtor’s wages, as long as the debtor is working more than 30 hours a week and earning more than minimum wage.
- For those who have received notice of garnishment, there is very little legal room for appeal. There is no provision in Kansas statutes that allows debtors to claim economic hardship as a way to avoid paying their debt. (Garnishments can stop when a patient declares bankruptcy.)
- Some sources of income cannot be garnished. These include but are not limited to: Social Security disability and retirement benefits, Supplemental Security Income, veterans benefits, and certain pension benefits and retirement funds.
- Assuming a defendant’s income is not exempt, interest, penalties and court costs can all be applied to a debt and collected through garnishment.
- Unless otherwise stated in a contract, the creditor can charge up to 10% interest during the period before a judgment is entered, and up to 12% after the judgment is entered.
Perhaps the most perilous threat a defendant can face is up to 30 days in jail. Here’s how that can happen:
Once a judgment is entered, the defendant has 14 days to pay the judgement. If it’s not paid in full, the creditor can begin garnishing wages, but only if lawyers know where the defendant works or banks. Often, creditors don’t have this information. Kansas law allows them to request that defendants appear in court to provide it. If the judge signs off on this request, defendants typically have about 30 days to appear in court, where they must tell the judge under oath where they work and bank.
If defendants fail to appear, the creditors’ attorneys can file a citation of contempt. The judge must sign off on this request, too. Once that happens, the creditors’ attorneys are responsible for making sure the defendant is personally served the contempt citation and ordered to appear in court. Vokins says he also requires the attorneys to spell out the consequence for not appearing – namely, that a warrant may be issued for their arrest. Once Vokins signs off on that warrant, he sets a bond for $250, an amount that can double at his discretion if a defendant fails to appear again.
“I want language in there that failure to appear may result in a bench warrant for your arrest,” he says. “I want debtors to have notice of the consequences. Nothing in Kansas law requires that. It’s my policy.”
The practice of issuing bench warrants is common, as Law360’s Access to Justice newsletter detailed in a February story. Although the U.S. outlawed debtors’ prisons in 1833 and the U.S. Supreme Court ruled in 1983 that jailing people over debt is unconstitutional, the American Civil Liberties Union counts 44 states that allow the arrest of someone who fails to appear in court after a creditor wins a judgment against them or who doesn’t provide that creditor with information about their finances.
Vokins objects to criticisms that ordering jail time could effectively be tantamount to sending the defendant to “debtors’ prison.” The defendant is facing jail time for failing to obey a court order, not because of the debt, he stressed. And that jail time is something that’s spelled out in Kansas statutes.
“The judge doesn’t make the law; the legislators make the law,” he says. “The judges follow the law.”
The law also allows Vokins to apply the bond money to the judgment that defendants owe.
“I have the discretion that rather than issuing a fine against the judgment debtor on the contempt citation and the state of Kansas retaining that bond money, I order the bond applied to the judgment,” Vokins states. “That way the judgment creditor gets some money and the judgment debtor gets the credit, or reduction off of the outstanding balance owed on the judgment.”
Michael Rapp of Stecklein & Rapp, a law firm in Kansas City with offices in Kansas and Missouri that specializes in consumer protection, has appeared in Vokins’ court a number of times. He has handled some medical debt cases, though most of those have focused on individuals whose debt is related to care received for a personal injury.
Like Johnson with Kansas Legal Services, Rapp says that defendants severely limit their options when they admit in court that they owe the money their creditors say they owe. “Once you raise your hand, it’s over,” he says. “You’ve admitted to everything they say. You’ve 100% surrendered. There are no defenses left.”
Rapp’s advice to defendants in medical debt cases? Don’t initially admit to the debt. He says that there’s always the possibility that a defendant can argue that a hospital’s bill is not reasonable. “Is it customary billing? If I’m uninsured, am I being charged a higher rate? Are they charging me more than someone else? If I negotiated in cash, would it be a lesser amount?”
Defendants can also argue the medical necessity of the procedure they received, or that someone else should have paid the bill, or that they did not receive charity care they were eligible for. But most defendants never receive legal advice before they appear in court.
Confiscating bail money helps attorneys collect on unpaid debts. But it raises concerns in Rapp’s view. “Reasonable minds can disagree, but turning a civil contract issue into a criminal issue needs to be done with extreme caution.”
Collections attorneys, Rapp says, can resort to a number of tools to get the information they need before requesting a bench warrant – and judges should ask them to use those tools. Credit reports can yield valuable information, as can skip traces, which can help determine a person’s whereabouts. “What searching have they done before using the coercive force of the government?” he asks.
Issuing a bench warrant, Rapp says, is especially problematic in light of the fact that many defendants who end up in jail don’t make much money. “The system should not be set up to victimize the poorest among us,” he says. “And that’s the frustrating part.”
Outside of Emergency Medicine Care, though, it’s been exceedingly rare for providers associated with other major Kansas City health systems to have cases in which bench warrants are issued. Spokeswomen for the University of Kansas Health System and AdventHealth Shawnee Mission say their systems do not engage in that level of collection action. Spokeswomen for Saint Luke’s Health System of Kansas City and Overland Park Regional Medical Center did not reply to messages seeking comment.
The Journal reviewed 944 uncontested limited action judgments involving those four hospitals in Johnson County District Court between 2014 and 2019. It found just one instance where the record indicates that the judge issued a bench warrant. But online journal entries don’t show who requested the warrant and whether it was ever executed.

Pandemic takes a financial toll
The pandemic and its devastating economic effects, however, add another wrinkle to the tale. When hospitals stopped providing nonemergency care to prepare for a surge of COVID-19 patients, it caused budgets to tank almost universally.
Citing figures from the American Hospital Association, The New York Times reported that hospitals are losing an estimated $50 billion a month. Hospitals across the country reported seeing 40% to 70% fewer patients from late March through early May. Furthermore, more than 134,000 hospital employees have lost their jobs, and several health systems in Kansas have announced layoffs or furloughs.
Olathe Health has not been spared. Jensen, the Olathe Health spokesman, says that compared with last year, the system has seen surgeries drop 63%, cath lab procedures decline 51%, primary care visits drop 43%, emergency visits decline 39%, and overall hospital admissions and observations are down 41%.
Federal funding to help offset the impact of the coronavirus has come in the form of $5 million in federal relief to Olathe Medical Center and $800,000 for the Olathe Health Physicians, an associated nonprofit. But the aid only offsets about 20% of the hospital’s losses, Jensen says, and since losses are continuing, the percentage it covers will shrink as the pandemic and the economic challenges it has created continue.
To weather the storm, the health system has drawn on reserve funds, reduced executive compensation, initiated a hiring freeze with minimal exceptions and delayed or eliminated non-critical capital and non-labor expenses. In June, it also put in place a voluntary retirement program with enhanced severance and health benefits that 115 associates and providers have signed up for. A functional realignment has trimmed the positions of another 33 associates, although some may stay with the organization in other roles.
“These are difficult decisions, and they are not being taken lightly,” Jensen says. “We believe the resulting financial impact will help us better position ourselves for continuing our mission as a not-for-profit health care provider. I continue to be inspired by our associates’ and providers’ commitment to caring for our patients and keeping our communities safe during this uncertain time.”
Other health care systems face similar challenges.
At AdventHealth Shawnee Mission, which has received about $10 million in federal relief payments, government aid has only partially offset significant losses in revenue from the cancellation of elective and outpatient procedures during stay-at-home orders, spokeswoman Morgan Shandler says.
“We are now reopening our needed health care services to our community, but our surgery, outpatient services and emergency visits are still not at pre-pandemic volumes,” she says.
While AdventHealth Shawnee Mission has not furloughed or laid off staff, the health system has several cost recovery initiatives, including a pause in hiring. Some team members have been deployed into new roles, such as COVID-19 screening and testing, Shandler says.
Despite those financial challenges, the health system also implemented new practices to extend “financial grace” to struggling patients. Those changes include extending the validity of financial assistance applications from six months to 12 months, offering a 30-day payment grace period to patients who inform the hospital that they’ve been negatively impacted by COVID-19, increasing payment plan time frames from 24 to 36 months, lowering the minimum monthly payment to $25, and directing bad debt account management vendors to allow for flexibility in payment plan terms and extend grace around late or overdue payment.
“We understand how challenging these times can be financially and how stressful financial pressures can be for our patients and their families. These emergency financial assistance procedures are intended to help alleviate those challenges,” Shandler says.
The University of Kansas Health System has received about $67 million in federal provider aid for its Kansas City metro operations, says Doug Gaston, senior vice president and chief financial officer. But that only covers about half of the nearly $120 million the system lost between March and May. The system decided not to furlough staff, Gaston says, because it needs that workforce on hand to help increase revenue as patients return.
In all, the federal government has provided at least $175 billion in relief funds to hospitals and other health care providers on the front lines of responding to the coronavirus through the CARES Act and the Paycheck Protection Program as well as the Health Care Enhancement Act. About $694 million of that funding has flowed to Kansas providers.
Despite that aid, the health care sector faces significant challenges in trying to bounce back. An increase in unemployed workers means fewer prospective patients with health insurance, who are more profitable to serve than patients on government programs such as Medicaid.
“We’re watching this really closely, because we don’t know if we’re going to see a shift in that payer mix,” says Colette Lasack, vice president of revenue cycle operations at the KU Health System. “We expect that we’re probably going to see more patients without insurance. But depending on their situation, some of those folks will also be eligible for the (ACA) marketplace plans where they might not have before.”
The financial pressure from the pandemic is likely to put more pressure on hospitals that depend more heavily on privately insured patients, The New York Times has reported. According to its IRS filings, Olathe Medical Center at present derives a very small percentage of its overall revenues from patients on Medicaid.
‘A hypercompetitive environment’
Olathe Medical Center’s legal activity has taken place against the backdrop of increasingly competitive business environments for health systems.
Olathe Health is a regional health network that serves southern Johnson County, and Miami, Linn and Franklin counties. In addition to Olathe Medical Center, it also includes Miami County Medical Center and the 40 family care and specialty clinics of Olathe Health Physicians. But it’s southern Johnson County where a number of health systems are competing to win the business of wealthy, well-insured patients using top-flight amenities.
The Kansas City Business Journal ranked Olathe Medical Center 10th in admissions among acute care general hospitals in the metro area with nearly 12,000 in 2017. The newspaper ranked it eighth in revenue, but the hospital is much smaller than several of the billion-dollar behemoth systems expanding in the region.
Jim Dockins, associate professor of management at the Rockhurst University College of Business, Influence and Information Analysis in Kansas City, Missouri, notes at least four other hospital chains have been adding beds, clinics and free-standing emergency rooms in southern Johnson County even as poorer neighborhoods in Wyandotte County and across the state line in Missouri go underserved.
“This is indeed a hypercompetitive environment,” Dockins says. “Everybody builds houses on the edges of town where it’s cheaper, and the hospitals tend to migrate toward the peripheries, because typically most people that are out there building and buying houses are going to have insurance.”
Keeping revenues up is likely on the minds of Olathe Health officials, Dockins says, especially after its recent $100 million expansion, funded in part by bonds issued by the city of Olathe.
“If you look at the amount of debt that they assumed over the past 10 years with their ongoing building program, I think that puts tremendous pressure on their bottom line,” says Dockins.
Prior to the pandemic, Olathe Medical Center generally reported positive net incomes overall. In its five most recent filings available from the IRS, the nonprofit hospital reported collecting at least $40 million more in revenues than it spent in each year between 2013 and 2017. Miami County Medical Center reported positive net incomes between $1.5 million and $4 million over the past six years. The Olathe Health Physicians group has reported annual losses ranging from $23 million to $32 million. The expenses associated with Olathe Health System, a fourth nonprofit entity, primarily have to do with management of the system.
According to hospital community benefit reports, spending on charity care and means-tested government programs generally went up across the system, rising from $11.8 million to $12.9 million from 2013 to 2018.
The hospital’s IRS filings also indicated that its aid to patients has been shifting away from direct financial assistance at cost to covering unreimbursed charges through Medicaid. In 2013, Olathe Medical Center and Miami County Medical Center combined to spend $5.3 million on financial assistance at cost but, by 2017, that figure had fallen to $4.2 million. The hospital was asked to provide 2018 figures but did not respond.
The decrease in direct financial assistance coincided with a drop in its eligibility level for free care from 200% of the federal poverty level to 150% of the federal poverty level between 2015 and 2016, according to IRS filings. Such changes are not uncommon. In the years since the ACA passed, Kaiser Health News reports that nonprofit hospitals around the country have been offering significantly less free and discounted care, often on the basis that they have fewer uninsured patients. But reductions generally occur in states that expanded Medicaid.
Olathe Medical Center does provide 80% discounts for households at 151% to 200% of the federal poverty level, 65% discounts for households at 201% to 300% of federal poverty level and discounts for households above 300% of federal poverty level on a case-by-case basis for extraordinary medical expenses.
Its own reports indicate that Olathe Medical Center is often trying to collect on debts from patients who should actually be receiving aid. Like most Johnson County hospitals, Olathe Medical Center used to report little or no bad debt from patients eligible for financial assistance under its policies. However, in 2016 and 2017, 90% and 75% of its bad debt came from patients who were eligible for financial assistance. The hospital’s filings indicated that the biggest reason for the bad debt is that eligible patients didn’t apply.
Nonprofit hospitals are required not only to provide financial assistance but also to take steps to make sure patients know that it’s available. To adequately publicize financial assistance policies under IRS regulations, nonprofit hospitals must make the policy and application for assistance widely available on the web. They are also required to provide paper copies upon request and without charge, both by mail and in public locations in the hospital, including the emergency room and admissions areas. Other requirements include notifying members of the community who are most likely to require financial assistance about the policy as well as individuals who receive care at the hospital.
Olathe Medical Center says it offers several different programs to assist patients in paying their bills, including assistance obtaining public health insurance (if eligible), providing charity care (financial assistance) or establishing a payment plan through CarePayment.
Hospital officials did not provide any additional explanation for why a high percentage of patients are not making use of financial assistance they should be eligible for.
Mark Rukavina, business development manager at Community Catalyst’s Center for Consumer Engagement in Health Innovation, a national advocacy organization, says Olathe Medical Center’s high bad debt percentages in 2016 and 2017 are worth noting.
There could be a variety of reasons why a hospital is unable to reach eligible patients, he says.
“People may be embarrassed,” Rukavina says. “They don’t fully exercise their rights because of that. Just because of the mere fact that they get sick, which is something none of us have control of. Hospitals have an obligation to inform patients. They have an obligation to follow their policies, and patients bear some responsibility as well. But something is awry with those kind of percentages.”

Dealing with patients ‘up front’
Olathe Medical Center officials said that all patients are kept informed of all financial assistance opportunities available to them.
“Multiple billing statements are mailed over the course of 90 days after the date of discharge to the last known mailing address,” the hospital said in a statement. “Each billing statement contains a visible notice of the availability of and information about how to apply for financial assistance. The patient’s account is then provided to CarePayment to attempt to set up a payment plan. If no plan or contact is made, the patient is then sent a letter informing them their account is being sent to a collection agency for nonpayment. The letter outlines the possible collection actions that may follow if payment is not arranged. For a successful financial arrangement, it’s reliant on the patient to communicate with the company providing the assistance.”
Olathe Health officials say they’ve set their sights on encouraging the Legislature to expand Medicaid as a way to reduce the burden of medical debt for their patients. They cite a worsening insurance environment for patients as being at the core of the problem.
“Unfortunately, as you can see from national trends,” the hospital’s statement said, “the number of uninsured and underinsured patients in America continues to increase. According to the U.S. Census Bureau, 27.5 million Americans did not have health insurance in 2018. The rate of uninsured Americans recently hit its highest rate since 2014. In addition, many Americans are underinsured because of higher deductibles and changes in insurance plans, or do not have access to Medicare or Medicaid.
“We are actively trying to help improve access and coverage in our state. Last year, Olathe Health hosted leaders from both parties (Governor Laura Kelly and Senator Jim Denning) to discuss Medicaid expansion in Kansas and the role of nonprofit hospitals in our community.”
Some critics of aggressive medical debt collections say there are much more effective ways to deal with unpaid patient debt than by suing, coercing payment plans and garnishing wages.
While garnishment might be a legal way for medical providers and other creditors to collect debt, the approach carries plenty of downsides, says Simon Sandoval-Moshenberg, legal director for the immigrant advocacy program at the Legal Aid Justice Center in Virginia, which provides legal services and advocates for low-income individuals.
Because of limits on how much a patient’s paycheck can be garnished, it can often take a long time for someone to make good on a judgment, especially if their bill is accumulating interest as they attempt to pay it off. Depending on how much a person makes, there’s a chance that it might even be increasing as the result of a garnishment, Sandoval-Moshenberg says.
The revenue from the garnishment doesn’t do much to help the hospital’s bottom line, but it can be a massive hit for a debtor who works for modest wages.
“Low-income people tend to use the nontimely payment of bills as almost a form of credit to get them through emergency situations,” Sandoval-Moshenberg says. “But it’s one of the most expensive forms of credit because of the interest and late fees.”
Rather than trying to collect whatever they can get right away, creditors might be better served to take a wait-and-see approach, he says.
“It is taking people who are in a financial hole and it is making it much more difficult for them to start climbing out of the hole,” Sandoval-Moshenberg says of garnishments.
Compared with Olathe Medical Center, most of the hospital’s nearby competitors are more generous with financial assistance and report being proactive at ensuring the patients who are eligible for financial assistance actually receive it. AdventHealth Shawnee Mission and the University of Kansas Health System both offer free care to households who earn up to 200% of the federal poverty level, which amounts to about $52,000 for a family of four.
The Saint Luke’s Health System offers free charity care to households that make up to 133% of the federal poverty level for unscheduled admissions. Patients making 134% to 200% of the federal poverty level have the responsibility for making a $700 copay per admission while those making 201% to 300% of the federal poverty level are responsible for a $1,500 co-pay.
Partially as a result of spending less on direct financial assistance and Medicaid, Olathe Medical Center also reports providing less benefit to the community than neighboring nonprofit hospitals. About 4.48% of its total operating expenses were spent on community benefits in 2017, less than AdventHealth Shawnee Mission (6.51%) and Saint Luke’s Hospital of Kansas City (9.89%), but more than Saint Luke’s South in Johnson County (2.67%).
A recent study in Inquiry: A Journal of Health Care Organization, Provision and Financing found that the average value of a nonprofit hospital tax exemption is 5.9% of total expenses, while the average level of total community benefits is 7.6% of expenses. At least one-third of all nonprofit hospitals receive more benefits from their tax exemptions than they provide in community benefits. But that study uses broader sets of data than are found in IRS filings.
Olathe Med’s nearby competitors also tend to be far less likely to try to collect unpaid bills from patients who should be eligible for financial assistance. In 2017, before it changed its name, Shawnee Mission Medical Center reported that just 1.68% of its bad debt was attributable to patients eligible for its financial assistance policy. Saint Luke’s reported that 0% of its bad debt came from patients eligible for financial assistance.
In their filings with the IRS, metro area hospitals describe the special measures they take to make sure patients who are eligible receive financial assistance. However, few were willing to talk in more detail about their financial assistance policies, how they ensure that patients use them, and their policies and procedures for collecting unpaid bills.
Spokeswomen for Saint Luke’s, Children’s Mercy Kansas City and Overland Park Regional Medical Center did not respond to multiple requests from The Journal for information about their collection and financial assistance policies.
The KU Health System did make one of its administrators available to be interviewed. Lasack, vice president of revenue cycle operations, says the system prioritizes being fair and consistent across its patient base and works to confirm the income of patients, to understand the circumstances they face and to exhaust all avenues of coverage before trying to collect on a bill.
The health system, which provides about 13% of the $96.2 million it spends on uncompensated care to Johnson County patients, has a team of 40-plus financial counselors and an outside contractor to work with patients to determine what they are eligible to receive.
Like Olathe Health, the KU Health System and related entities sue patients and seek garnishments in Johnson County. Over the past six years, it has sought about 40 garnishments each year to collect on uncontested judgments compared with the 130 and 360 garnishments that have been sought annually by Olathe Health System entities and Emergency Medicine Care, respectively.
When the system does allow a credit agency to take patients to court on its behalf, it is usually for amounts above $750, KU Health System spokeswoman Jill Chadwick says. The system also requires a double-check on any past charity care, to make sure the patient is not still in need, to consider whether the patient is receiving ongoing treatments and to take stock of any unusual circumstances. The past bad-debt history of the patient and whether they cooperated or not might also be considered.
Lasack says the KU Health System hasn’t changed any policies as a result of the pandemic. Since March it has worked to open lines of communication with patients experiencing layoffs, furloughs and reduced hours and provide flexibility.
“We had patients starting to call us that were in a very different financial situation than they were in the week before,” Lasack says. “We have worked really hard to be flexible with our patients, whether that means extending their payment plans, whether that means skipping a payment this month. Call us, let us know your situation. Really that’s what patients were asking for: ‘Work with us because we don’t know.’ Just like we didn’t know how long this was going to go on.”
Being able to have an open dialogue, where patients feel comfortable contacting the hospital and feel like their individual situations are being taken into consideration, is a crucial part of the process. In short, the hope is to move away from situations where patients feel surprised and hospitals feel obligated to chase down unpaid bills.
“Where we need to move as an industry is, ‘How do we have that transparency up front and educate that patient about what to expect?’” Lasack says.
Many of the patients sued by Olathe Medical Center and Emergency Medicine Care told The Journal that they wanted to pay their bills. They understood that nonprofit hospitals need to have sufficient revenue to operate. Hospital officials, for their part, acknowledge the challenges patients face and say they’re making changes to help, even as their collection lawsuits and garnishments vastly outstrip those of neighboring hospitals.
Like so many nonprofit hospitals, Olathe Medical Center describes its mission in lofty, egalitarian terms: “To help people through healing, health and happiness.” The hospital and emergency room providers contend they live out this mission through their care of patients. But The Journal also asked hospital officials how they saw their collection lawsuits and garnishments fitting with that mission.
It was one of several questions hospital officials never answered.
Maya Miller, engagement reporter at ProPublica, contributed to this story by providing frequent advice and insight. If you have been arrested after missing court for unpaid medical bills or have been sued by a hospital, doctor or other medical institution, please share your experiences with ProPublica here. ProPublica shares these tips with local reporters such as The Journal. Tips to ProPublica launched the investigation that led to this story.



